Why sleep has restorative—or damaging—effects on cognition and brain health has been an enduring mystery in biology. Researchers think cerebrospinal fluid (CSF) may flush toxic waste out, “cleaning” the brain and studies have shown that garbage clearance is hugely improved during sleep. They were not sure exactly how all this works, however, or why it should be so enhanced during sleep.
One aspect of sleep that is well understood is how the slow electrical oscillations (or “slow waves”) that characterise deep, non-REM sleep contribute to memory consolidation, the process whereby new memories are transferred into long-term storage. A new study, from a team led by neuroscientist Laura Lewis of Boston University, now gives insight into what drives CSF flow through the brain, suggesting that the same slow waves that coordinate memory consolidation drive oscillations in blood flow and CSF in the brain.

The work has implications for understanding the relations between sleep disturbance and psychiatric and neurodegenerative conditions, and may even point to new approaches to diagnosis and treatment. The study discovered that there are large waves of CSF that appear in the brain only during sleep. This effect is striking, and scientists are also interested in what it means for maintaining brain health, especially in disorders such as Alzheimer’s disease.
In the study, published on in Science, the team set out to investigate how the dynamics of CSF flow changes during sleep, and how this might relate to alterations in brain blood flow and electrical activity.
The researchers used electroencephalography (EEG) to monitor the brain waves of 13 sleeping healthy adults, while also using a cutting-edge, “accelerated” fMRI technique to capture faster changes than standard fMRI can manage. That allowed for the measurement of both blood-oxygenation changes (which indicate blood flowing to electrically active, oxygen-hungry regions) and CSF flows. The latter was only possible due to a flaw in this method that means any newly arriving fluid (not just oxygenated blood) lights up in the image. This turned out to be critical, because it turned out that these were coupled to each other in a way that would never have been seen if we blood, CSF and electrical activity weren’t measured simultaneously.
What the team found was that the slow waves seen in non-REM sleep occur in lockstep with changes in both blood flow and CSF. Just because things occur together doesn’t necessarily mean one causes the other, but the team also built a computer model incorporating what we know about the physics linking these processes, which predicted that slow waves would have just these kinds of effects on blood and CSF. What seems to be happening is that as brain activity alters blood flow, this reduces the volume of blood in the brain, and because the brain is a closed vessel, CSF flows in to fill the space. Electrical activity drives blood flow changes, that then drive CSF changes.
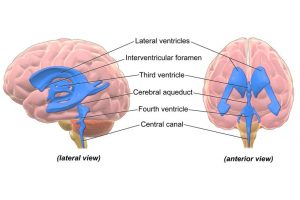 The team measured this CSF inflow going into the fourth ventricle, one of four fluid-filled cavities involved in producing CSF (by filtering blood plasma) and circulating it around the brain. As CSF usually flows out of the fourth ventricle, this suggests a “pulsatile” flow, like a wave. This pushes CSF around the ventricles and into spaces between membranes surrounding the brain and spinal cord, called the meninges, where it mixes with “interstitial fluid” within the brain to carry away toxic waste products.
The team measured this CSF inflow going into the fourth ventricle, one of four fluid-filled cavities involved in producing CSF (by filtering blood plasma) and circulating it around the brain. As CSF usually flows out of the fourth ventricle, this suggests a “pulsatile” flow, like a wave. This pushes CSF around the ventricles and into spaces between membranes surrounding the brain and spinal cord, called the meninges, where it mixes with “interstitial fluid” within the brain to carry away toxic waste products.
As slow waves are important for memory consolidation, this links two disparate functions of sleep. What’s exciting about this is it’s combining features of brain function that people don’t normally think of as connected. It isn’t obvious things had to be this way, but it may represent an example of nature being efficient. It’s a matter of nature not dividing tasks between higher level and lower level, like how you run a company, where you have a boss making decisions and cleaning people coming in. In biology, it’s everybody contributing, as it makes more sense.
The findings have implications for neurodegenerative diseases, which are thought to be caused by build-up of toxic proteins in the brain, such as amyloid-Beta in Alzheimer’s disease. Previous research has shown that amyloid-Beta is cleared more efficiently during sleep, which is often disrupted in patients. Disturbances in slow-wave sleep also often accompany aging, which may be linked to cognitive decline.
We know that people with Alzheimer’s have fewer slow waves, so it could be that they also have fewer CSF waves. These studies have to be carried out in older adults and patient populations, to understand what this might mean for those disorders. Sleep disturbance is also a feature of many psychiatric disorders, from depression to schizophrenia. Different electrical signatures of sleep are disrupted in different psychiatric conditions. So this will be something to watch out for in the coming years.
The team next hope to nail down whether electrical oscillations truly do cause the changes they observed in CSF flow, by experimentally manipulating brain activity. It may ultimately be possible to use electromagnetic stimulation to influence brain waves as a treatment for brain disorders. Researchers have already seen encouraging results of this approach in mice, and these findings may help explain why. Another potential application may come from assessing whether changes in CSF flows can serve as a diagnostic marker for some of these conditions.
It seems like things the brain is doing during sleep are related to each other in surprising ways. Maybe the most important take-home message is that sleep is a serious thing. You need to sleep to keep a healthy brain because it links electrical activity to a practical housekeeping function.
REFERENCES:
Coupled electrophysiological, hemodynamic, and cerebrospinal fluid oscillations in human sleep. Nina E. Fultz et al. Science 01 Nov 2019: Vol. 366, Issue 6465, pp. 628-631.
